Click
here -> to return to the opening page or to
exit
Supplies Database
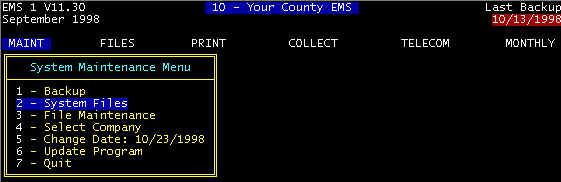
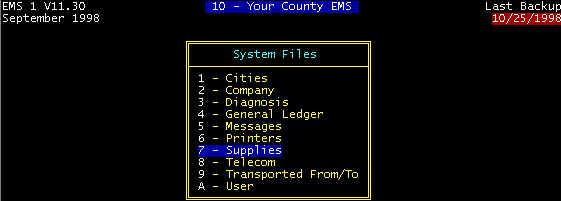
Menu Path: MAINT/System Files/Supplies
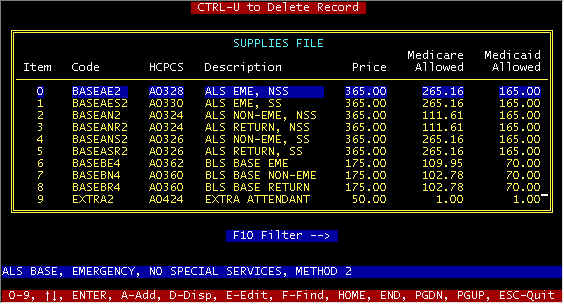
The SUPPLY database allows you to establish your charges and descriptions such that when posting charges after entering a trip ticket, that correct charges, HCPCS codes, and descriptions are extracted and attached to the invoice for filing claims. Additionally, after entering a trip ticket, the computer will display a charge screen for acceptable Medicare charges, based on data entered into the invoice screen (from the trip ticket).
Your Supplies Screen determines Medicare/Medicaid
charges that will be billed
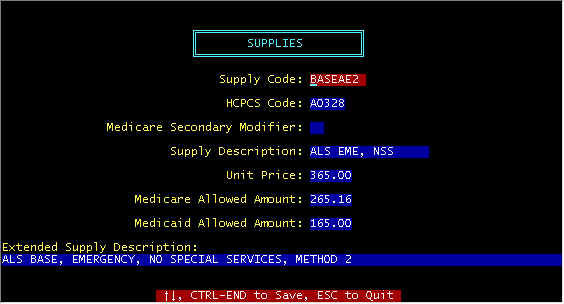
The SUPPLY database file is a supporting file to invoices, in that data (including all prices) from this file are extracted during the time charges are being posted to invoices. HCPCS codes and descriptions are directly from Medicare to reduce the possibilities of claims rejections. Most insurance companies require these codes and Medicare requires them on all electronic claims. The SUPPLIES file is accessed three ways: ŒAfter adding a new invoice, certain charges are determined from invoice data fields, for example if this is an ALS call, a charge record is created for this invoice and a BASEA charge is automatically inserted (this charge record is completed by posting charges), during POSTING charges data entry, at which time the HCPCS codes, supplies descriptions, and price are copied to the charges screen (and file); and Žmanual add/edit/display from the menu selections as shown. CTRL-U to Delete Record -- the highlighted record will be deleted. Code -- There are two categories of codes: · codes that should not be changed because these are used by the program, and depend upon the exact characters, and · codes that are added per provider preference -- for example local codes allowed by certain carriers (and possibly not by all carriers); these may be disposable supplies such as certain IV drugs, etc. Note that codes ending in 1 are Method 1 codes, 2 = Method 2, etc. Codes used depend upon the billing method(s) in use by your carrier, and will vary from state to state. Billing Methods 1-4 are discussed on an immediately following page in this section of your manual. HCPCS -- These codes are supplied by Medicare, and codes not compatible with your carrier may be rejected. However, certain codes (listed on a following page) includes the new codes universally accepted by Medicare effective beginning January 1, 1995., but there may be additional Local Codes for your area. Description -- An abbreviated description is shown in the main screen, but the complete description of the highlighted code is shown in the lower part of the screen. Price -- This is the price you charge. Your Supplies Screen determines what is will be billed to Medicare/Medicaid. Posting charges that are not allowed is OK, but these will not be included when filing claims as described below. Medicare Allowed -- This is what is listed on your EOMB’s as "Allowed". This is the lowest number in your fee screen, usually your Customary IIC. You will be reimbursed 80% of this value, and you will bill the other 20% to co-pay. The difference between what you charge (price) and the Medicare allowed must be written off as Medicare Contractual, and is uncollectable. There are two uses of this amount: å any time this value is zero (0) the billing system will not include when you bill Medicare (but will be included on other claims), å and this amount is used in computing your Medicare expected payment report. Medicaid Allowed -- similar to Medicare (above). F10-> Filter -- Entering a string of characters will generate a new window showing codes for which this matching string appears in the description fields. 0-9, ¯ , HOME, END, PGDN, PGUP -- These reposition the cursor and/of screen position, with home jumping to the beginning of file, end to end of file. ESC-Escape -- return to the previous menu, abort any key entry. F-Find -- As previously described, F10 searches for a string-match in the description field; similarly, F-Find searches the Code field. A-Add, E-Edit, D-Display -- displays the detail supply screen shown below for the highlighted supply -- field descriptions were previously described immediately above. When posting charges, a short code entry will reference supply codes in the SUPPLIES file and extract: the corresponding Œsupplies description, HCPCS code, and Žprice. If the exact code is not entered, a window of codes as shown above in the main screen will be displayed for either exact selection or searching. Supply Code -- Used internally. Some codes should not be changed, such as base rates, mileage, etc. since the computer uses these to assist in posting charges. HCPCS Code -- defined by Medicare Medicare Secondary Modifier -- Used by Tennessee for itemized drugs (see next page). Supply Description -- Abbreviated to what can be filed with electronic/paper claims -- Note that for Tennessee, Mileage should include "Out of County" Unit Price -- Amount that you charge. Medicare/Medicaid Allowed Amount -- If zero, this charge will not be billed. Otherwise this is the amount "Allowed" on your EOB’s. The amount here is used for the "Expected Payment Report". Extended Supply Description -- This is an extension for more details for the Supply Description (above), and is used only for your benefit.
CTRL-END / ESC -- Holding the Ctrl key down and tapping the END key will save the current screen, whereas the ESC(ape) key will abort, leaving the screen data to what it was prior to the current screen.
A similar screen to that shown above is displayed during posting charges so that base rate HCPCS codes can be differentiated between special and no special services, at which a Y(es) / N(o) selection can be made to effect this differentiation. |